Knowledge about Medicare-for-All Remains Low and People’s Views Differ on What the Policy Would Do
Almost half (46 percent) of adults say they have not heard anything about a proposal called “Medicare-for-All”.
CHICAGO, Jan. 24, 2019 — Forty-six percent of adults report that they have not heard about a health policy proposal called “Medicare-for-All,” according to a new AmeriSpeak® Spotlight on Health survey from NORC at the University of Chicago. Forty percent say they have heard some talk about Medicare-for-All, and 13 percent say they have heard a lot about it.
During the 2018 elections, many Democratic candidates and seated members of Congress came out in support of a Medicare-for-All plan. However, as the results of the survey make clear, the idea means different things to different people, and most politicians have not defined the specific policy parameters they support. In fact, at least seven bills have been introduced in Congress to expand Medicare coverage to more people. These proposals range from extending mandatory Medicare coverage to all Americans with no cost sharing (e.g., S.1804 introduced by Senator Bernie Sanders) to giving individuals age 55 and older the option to buy into the Medicare program to access benefits as they exist today (e.g., S.1742 introduced by Senator Debbie Stabenow).
“'Medicare-for-All’ is a term that means something different to everyone, which makes it hard for the public to understand how such a program would work,” said Caroline Pearson, senior fellow at NORC. “As the policy debate unfolds, politicians will need to coalesce around some key parameters of a Medicare-for-All proposal to help voters understand the impact.”
People are divided on how participation in a Medicare-for-All plan would work.
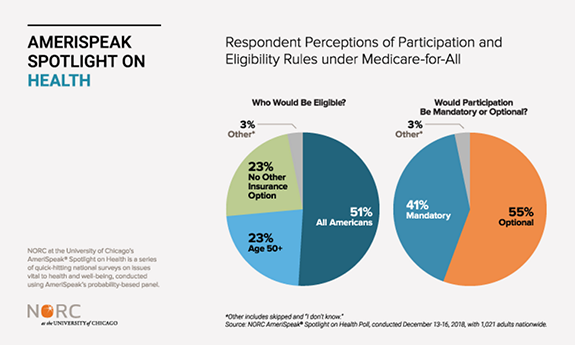
Two key questions that policymakers will need to decide when structuring a Medicare-for-All proposal are: 1) who will be eligible, and 2) will it be mandatory or optional for people to enroll. When asked who could participate in Medicare-for-All, survey respondents were divided. Among all adults who answered the survey, half (51 percent) thought Medicare-for-All would include all Americans, 23 percent believed the plan would include only those 50 years old and over, and another 23 percent thought the plan would only be available to people without other sources of insurance. When asked about whether people would be required to participate, 55 percent of all respondents thought that enrollment would be optional, whereas 41 percent believed it would be a mandatory program. Notably, these responses varied based on how much people had heard about Medicare-for-All as a policy (see chartpack for detailed results).
People generally believe Medicare-for-All would expand coverage and lower patient costs but that such a plan would increase overall U.S. spending on health care.
When asked what concerns them most about the health care system, people prioritized patient out-of-pocket costs followed by coverage for health care services (see chartpack). More people believed that Medicare-for-All would have a positive impact by reducing patient costs (49 percent) and expanding coverage for services (44 percent), compared to those who thought it would have a negative impact. One in five respondents did not think the policy would change patient costs or coverage. While respondents were somewhat less concerned about access to doctors and hospitals, they also believed a Medicare-for-All plan would improve access to these providers.
“People expect that Medicare-for-All will address the issues that matter most to them, namely reducing out-of-pocket costs and increasing breadth of coverage.” said Michelle Strollo, vice president at NORC. “At the same time, they seem to recognize that such benefits would come at a cost with a Medicare-for-All plan likely to drive up total U.S. health care spending.”
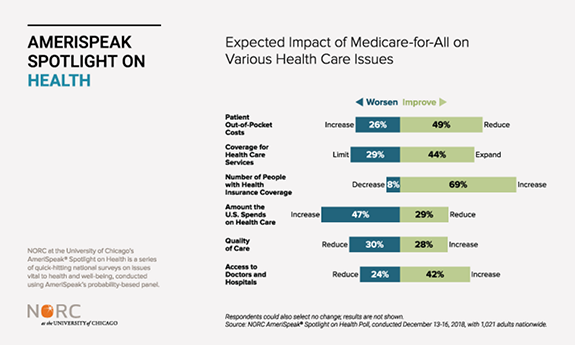
More than two-thirds of respondents think that a Medicare-for-All plan would increase the number of people with insurance (69 percent), compared to only 8 percent who think the number of people with insurance coverage would go down.
Notably, total spending is anticipated by many to get worse under Medicare-for-All. Forty-seven percent think that overall U.S. spending on health care would go up under Medicare-for-All, compared to 29 percent who think total spending would go down and 21 percent who believe spending would not change. When asked about quality of care, 30 percent of people said quality would get worse, 28 percent said quality would get better, and the largest group (39 percent) said it would not change.
Methodology
The self-funded poll was conducted between December 13 and 16, 2018, during a monthly Omnibus survey. It included 1,021 interviews with a nationally representative sample (margin of error +/- 4.26 percent) of adult Americans aged 18+ using the AmeriSpeak® Panel. AmeriSpeak is NORC’s probability-based panel designed to be representative of the U.S. household population. A comprehensive listing of all study questions, tabulations of top-level results for each question,
About the AmeriSpeak Spotlight on Health
NORC at the University of Chicago’s AmeriSpeak® Spotlight on Health is a series of quick-hitting national surveys on issues vital to health and well-being, conducted using AmeriSpeak’s probability-based panel.
About NORC at the University of Chicago
NORC at the University of Chicago conducts research and analysis that decision-makers trust. As a nonpartisan research organization and a pioneer in measuring and understanding the world, we have studied almost every aspect of the human experience and every major news event for more than eight decades. Today, we partner with government, corporate, and nonprofit clients around the world to provide the objectivity and expertise necessary to inform the critical decisions facing society.
Contact: For more information, please email press@norc.org or call (877) 832-0392.





